To Discourage Unnecessary Trips, Some Japanese Cities Have Started Charging for Non-Emergency Ambulance Rides
Japan has partially implemented new triage services via phone and online chatbots to limit ambulance use.

What’s new: As of June 1, 2024, the city of Matsusaka in Mie Prefecture (near Nagoya) began charging 7,700 yen (about US$50) if a patient is taken to the hospital by ambulance but is not admitted.
Zoom in: Matsusaka City says the fee is not technically a charge for the use of an ambulance. It is not collected by the city or the fire department and is, therefore, not a "payment.” What is being used is a system called "Selective Medical Treatment Fee," which is called sentei ryoyohi (選定療養費) in Japanese. This is a fee charged when a patient visits a hospital with 200 or more beds without a letter of introduction or shokaijo (紹介状) in Japanese1.
The three general hospitals in the city had not collected fees from patients transported by ambulance, but after consultation with the city and the fire department, they decided to collect 7,700 yen when a patient is transported by ambulance but not admitted to the hospital.
This is based on the existing system, and even in cases of minor illnesses, the fee is not applied to patients transported due to accidents. The final decision on whether to charge the fee is made by the hospital doctor.

Why it matters: Like many countries in Europe, such as France, Germany, Italy, and Spain, where ambulance rides to the hospital are free of charge to the patient2, ambulance transportation for patients experiencing a medical emergency are free in Japan.
Nationally, the volume of calls has become so high that the response time has now exceeded 10 minutes for the first time. This is literally a critical milestone because when a patient suffers cardiac arrest due to a heart condition, for example, survival becomes extremely difficult if the time exceeds 10 minutes without life-saving treatment.
The "Selective Medical Treatment Fee" was introduced to prevent the concentration of patients in general hospitals and to separate the roles of local clinics and other medical facilities. By charging a fee for minor illnesses, the city hopes to encourage local clinics and family doctors to consider the matter before calling an ambulance, thereby reducing the number of ambulance calls.

By the numbers: Japan's emergency medical services system is on the verge of becoming unsustainable.
Volume of Calls: According to the Fire and Disaster Management Agency of the Ministry of Internal Affairs and Communications, there were approximately 7.6 million ambulance calls nationwide last year. The number of ambulance dispatches reached a record high for the second year in a row.
Response Time Falling: The average time from the receipt of an emergency call to the arrival of an ambulance at the scene was 10.3 minutes, according to the latest data available at the end of last year. This is four minutes slower than 20 years ago, and the first time that this critical period has exceeded 10 minutes.
High Rate of Misuse: Some hospitals do not admit 60% of those brought to the hospital by ambulance. The Emergency Medical Center of Tosei Hospital in Seto City, Aichi Prefecture, has, for example, records showing that 60% of patients transported to the emergency room by ambulance do not need to be hospitalized. This statistic is not unusual. It is well known that ambulances in Japan are often diverted to other hospitals due to staffing shortages, lack of on-duty specialists, and communication problems. So one might theorize that the main reason for the high volume is inappropriate use, such as "I'm too drunk to walk" or "I thought the ambulance would be faster because there is a line at the emergency room." However, there are almost no such calls. The vast majority of people who called for an ambulance were anxious because they did not know what to do and simply thought it was better to be safe than sorry - especially since the service is still free for most of the country.

What they're saying: Local doctors say Covid may have increased health concerns and lowered the bar for calling an ambulance.
"Some people just come to the hospital in an ambulance with only a fever because they are worried. I thought the number of such cases would decrease after Covid subsided, but I am surprised that the number of such instances is actually increasing." - Dr. Toshihiko Ichihara, Director, Emergency Medical Center, Tosei Hospital, Seto City, Aichi Prefecture, Japan
Healthcare and firefighting professionals in Matsusaka decided that something had to be done to ensure the sustainability of their emergency response system, which is accessed by dialing 1193 in Japan.
"I believe that many citizens call for an ambulance when they are not sure whether they are suffering from a minor or serious illness and do not know what to do. I want people to call 119 without hesitation if they feel that their condition is different from usual. However, I would like people to take measures such as consulting their family doctor in advance or going to the hospital as soon as possible, rather than waiting until the last minute to call 119.” - Chikusa Itokawa, Section Chief, Matsusaka Area Wide-area Firefighting Union, Emergency Medical Services
Doctors at the hospitals served by the dispatch service realized that the system had reached its breaking point.
"As an emergency physician, I would like to accept and treat all patients. But if we continue to accept patients with minor illnesses without turning them away, there is a possibility that one day we will miss a seriously ill patient or not be able to treat them properly.” - Dr. Ichihara
The bottom line: With an aging population and fewer extended families living under one roof, many patients call an ambulance because they have no means of transportation. Ambulances are the only way to get to the hospital.

The other side: With the increasing number of elderly people living alone, there are many cases where a relative living far away calls for an ambulance to take their parent to the hospital, for example, but the patient refuses to be transported.
"I tried to explain strongly enough to convince the patient (to board my ambulance to go to the hospital), but he stubbornly refused. Since we were told that the patient had not deteriorated rapidly, we judged that the situation was not urgent and did not transport him to the hospital...There have been cases where we have tried for over an hour to persuade the patient to board the ambulance, but we were unable to transport him or her." - Paramedic Masataka Matsumoto, Deputy Chief of the Matsusaka Area Wide-area Firefighting Union, Emergency Medical Services
This mismatch of resources has become a strain on the entire system. Such "patients" unnecessarily burden the system and may prevent ambulances from reaching the injured or sick in time, prevent lives that could have been saved, or prevent early treatment.
What’s next: What should you do if you or a family member becomes ill and you are not sure whether to call an ambulance?
In many parts of the country, a free telephone triage consultation service is now available by dialing 7119 from any telephone. When you call this number, a nurse or other health care professional will ask you about your symptoms and determine whether it is appropriate to call an ambulance immediately, or whether you should simply see your doctor in the morning or as soon as possible without having to go to the hospital.
It is equivalent to NHS 111 in the UK, Patientenberatung 116 117 in Germany, and Healthdirect 1800 022 222 in Australia, for example.
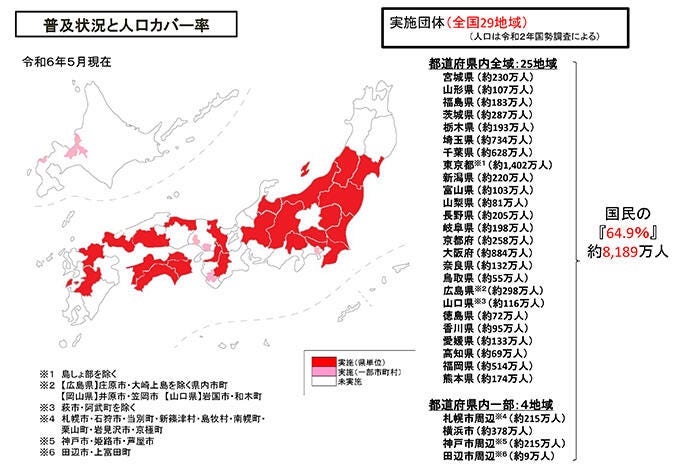
Currently, the #7119 service is available in 25 prefectures (out of 47) and 4 other major cities, covering an estimated 65% of the country's population.
In addition, people who live in areas where such telephone consultation is not yet available can take advantage of the free application Q-Support, which is called Qjo (Q助) in Japanese4. It is maintained by the Fire and Disaster Management Agency of the Ministry of Internal Affairs and Communications. Currently, only Japanese is available for both the mobile version and the website.
The first level of basic questions includes the following:
No breathing?
No pulse? Heart stopped?
Submerged (underwater)?
Feels cold? Shivering and shaking?
None of the above?
There are not too many more questions for the first 4 obvious emergencies. The suggested next step for "No pulse?" is, as you can imagine, to call 119 for immediate help. On the other hand, if you answer "None of the above?" you will be redirected to a series of additional questions.
Likely results are "Call an ambulance now" or "Go to a medical facility even though it is not an emergency."
Commentary: My only ambulance ride in Japan thus far was when I accompanied the unconscious teammate on one of my son's high school club soccer teams who had suffered a concussion after a mid-air collision with an opponent. Both players were trying to get a header but ended up knocking themselves out. The parents of my son’s teammate were both out of town, and I volunteered to ride in the ambulance and stay with the boy until one of his parents could get to the hospital. To spare you the suspense, my son's teammate made a full recovery.
The first thing that struck me about this experience was that it was a series of "hurry up and wait" maneuvers. After the ambulance arrived, we sat in the parking lot next to the soccer field for what seemed like an eternity. I kept thinking and asking, "Shouldn't we go to the nearest hospital right away?" It turned out that one of the paramedics had been on the phone for about 40 minutes trying to find a hospital that would take my son’s teammate and be able to do a CT scan. Of course, this was a Sunday evening on the far eastern edge of Tokyo. I later learned that the paramedic was turned down by four hospitals before he finally reached a place that would take the kid.
The next strange part of this experience was the trip to the hospital, which was a wild ride, mostly on the wrong side of the road with sirens blaring. It took us another 40 minutes to get to the hospital, which seemed way too long, especially in Tokyo.
While I ended up missing almost the entire soccer game, I did what any other parent would do and stayed at the hospital until the boy's mother arrived. Needless to say, the boy's parents and the soccer coach were grateful. In the end, everything turned out fine, and we all got to experience firsthand what it is like to use an ambulance in Japan.
Especially for accidents or obvious medical emergencies, no one should have to worry about calling an ambulance. Every second counts. But there is more of a gray area when the symptoms or circumstances are unclear. Given that Matsusaka city officials determined that their current system of providing emergency medical services was no longer sustainable, the novel use of "charging" for the Selective Medical Treatment Fee seems like a reasonable method of discouraging the unnecessary use of ambulances - especially in a country with such a large proportion of elderly people. I bet that other cities around the country will soon emulate Matsusaka.

What do you think? What do you think about the practice of charging for an ambulance ride? All answers are completely anonymous, even to the author.
Links to Japanese Sources: https://www3.nhk.or.jp/news/html/20240604/k10014466921000.html, https://hospitalsfile.doctorsfile.jp/reference_letter/, and https://www.fdma.go.jp/mission/enrichment/appropriate/appropriate006.html.
#ambulance #emergency #EmergencyMedicalCare #CarAccident #injury #illness #FireAndDisasterAgency #dementia #CriticalCare #paramedic #EMT #救急車 #救急医療 #交通事故 #けが #病気 #総務省消防庁 #119番通報 #高齢化 #認知症 #救命救急 #選定療養費 #7119番通報 #Q助 #救急救命士
The letter of introduction is used by primary care physicians who work at small, neighborhood clinics, for example, to provide patient information to referring departments and larger medical institutions. It contains detailed information about the patient's medical condition. Officially, it is called a "medical information form" or shinryo joho teikyosho (診療情報提供書) in Japanese. For example, if your primary care clinic diagnoses a suspected stroke and determines that detailed tests and advanced medical treatment are needed, you will be referred to a specialized neurologist or hospital. The referral letter is not a mere formality; it describes the patient's condition, medical history, test results, etc., and is used to facilitate cooperation between the family doctor and other medical institutions.
Even in countries where ambulance rides are free, there may be some exceptions. For example, if the ambulance is called for a non-emergency, the patient may be charged. In addition, some countries may have different rules for tourists and visitors.
In Japan, the three-digit emergency number is 119 (not 911 in the U.S., 999 in the U.K., or 112 in Europe).
Qjo is a play on the Japanese word kyujo (救助), which means rescue.






Sadly, it is clear to me that the strain on the ambulance service is yet another consequence of the deaths and injuries being caused by the covid so-called "vaccines." After the jabbing started, every time I went out I would see at least one ambulance on an emergency call every 30 minutes or so. Prior to the jabs, I seldom saw one.
According to a recent report by Japanese scientists, there were 115,799 “age-adjusted excess number of deaths” in 2022 after two-thirds of the Japanese population had received the third dose of COVID vaccine:
https://www.zerohedge.com/covid-19/excess-deaths-japan-hit-115000-following-3rd-covid-shot-new-study-explains-why
It is also great to see respected Japanese doctors, like Professor Masanori Fukushima and Professor Masayasu Inoue, blowing the whistle on the turbo-cancers and other serious harms being caused by the covid shots and demanding that the covid jabs be withdrawn from use/sale immediately:
https://www.aussie17.com/p/japan-vaccine-study-groups-press?utm_source=substack&utm_campaign=post_embed&utm_medium=web
https://www.aussie17.com/p/a-message-from-japan-to-the-world
This is undoubtedly the greatest crime against humanity during my lifetime, and the ambulance crisis is just one small symptom of it.
I wish they'd plaster the non-emergency number everywhere; it's not even listed on the nagging posters telling people how ambulances are being misused.